Abstract
Objective:
To determine if premedication and training level affect the success rates of neonatal intubations.
Study Design:
We retrospectively reviewed a hospital-approved neonatal intubation database from 2003 to 2010. Intubation success rate was defined as the number of successful intubations divided by the total number of attempts, and then compared by trainee’s experience level and the use of premedication. Premedication regimen included anticholinergic, analgesic and muscle relaxant agents.
Result:
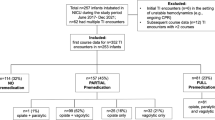
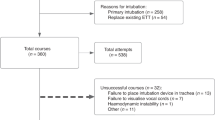
There were 169 trainees who completed 1071 successful intubations with 2694 attempts. The median success rate was 36% by all trainees, and improved with training level from 29% for pediatric trainees to 50% for neonatal trainees (P<0.001). Premedication was used in 58% of intubation attempts. The median success rate was double with premedication (43% versus 22%, P<0.001).
Conclusion:
Neonatal endotracheal intubation is a challenge for trainees. Intubation success rates progressively improve with experience. Premedication is associated with improved success rates for all training levels.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Kattwinkel J, Perlman JM, Aziz K, Colby C, Fairchild K, Gallagher J et al. Neonatal resuscitation: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Pediatrics 2010; 126 (5): e1400–e1413.
Bismilla Z, Finan E, McNamara PJ, LeBlanc V, Jefferies A, Whyte H . Failure of pediatric and neonatal trainees to meet Canadian Neonatal Resuscitation Program standards for neonatal intubation. J Perinatol 2010; 30 (3): 182–187.
Falck AJ, Escobedo MB, Baillargeon JG, Villard LG, Gunkel JH . Proficiency of pediatric residents in performing neonatal endotracheal intubation. Pediatrics 2003; 112 (6, Part 1): 1242–1247.
Leone TA, Rich W, Finer NN . Neonatal intubation: success of pediatric trainees. J Pediatr 2005; 146 (5): 638–641.
O'Donnell CP, Kamlin CO, Davis PG, Morley CJ . Endotracheal intubation attempts during neonatal resuscitation: success rates, duration, and adverse effects. Pediatrics 2006; 117 (1): e16–e21.
Kumar P, Denson SE, Mancuso TJ . Premedication for nonemergency endotracheal intubation in the neonate. Pediatrics 2010; 125 (3): 608–615.
Byrne E, MacKinnon R . Should premedication be used for semi-urgent or elective intubation in neonates? Arch Dis Child 2006; 91 (1): 79–83.
Bhutada A, Sahni R, Rastogi S, Wung JT . Randomised controlled trial of thiopental for intubation in neonates. Arch Dis Childhood Fetal Neonatal Edn 2000; 82 (1): F34–F37.
Friesen RH, Honda AT, Thieme RE . Changes in anterior fontanel pressure in preterm neonates during tracheal intubation. Anesth Analg 1987; 66 (9): 874–878.
Kelly MA, Finer NN . Nasotracheal intubation in the neonate: physiologic responses and effects of atropine and pancuronium. J Pediatr 1984; 105 (2): 303–309.
Marshall TA, Deeder R, Pai S, Berkowitz GP, Austin TL . Physiologic changes associated with endotracheal intubation in preterm infants. Crit Care Med 1984; 12 (6): 501–503.
Oei J, Hari R, Butha T, Lui K . Facilitation of neonatal nasotracheal intubation with premedication: a randomized controlled trial. J Paediatr Child Health 2002; 38 (2): 146–150.
Stow PJ, McLeod ME, Burrows FA, Creighton RE . Anterior fontanelle pressure responses to tracheal intubation in the awake and anaesthetized infant. Br J Anaesth 1988; 60 (2): 167–170.
Carbajal R, Eble B, Anand KJ . Premedication for tracheal intubation in neonates: confusion or controversy? Semin Perinatol 2007; 31 (5): 309–317.
Lago P . Premedication for non-emergency intubation in the neonate. Miner Pediatr 2010; 62 (3, Suppl 1): 61–63.
Shah V, Ohlsson A . The effectiveness of premedication for endotracheal intubation in mechanically ventilated neonates. A systematic review. Clin Perinatol 2002; 29 (3): 535–554.
Barrington K . Premedication for endotracheal intubation in the newborn infant. Paediatr Child Health 2011; 16 (3): 159–171.
Barrington KJ, Finer NN, Etches PC . Succinylcholine and atropine for premedication of the newborn infant before nasotracheal intubation: a randomized, controlled trial. Crit Care Med 1989; 17 (12): 1293–1296.
Bottor LT . Rapid sequence intubation in the neonate. Adv Neonatal Care 2009; 9 (3): 111–117.
Pokela ML, Koivisto M . Physiological changes, plasma beta-endorphin and cortisol responses to tracheal intubation in neonates. Acta Paediatr 1994; 83 (2): 151–156.
Roberts KD, Leone TA, Edwards WH, Rich WD, Finer NN . Premedication for nonemergent neonatal intubations: a randomized, controlled trial comparing atropine and fentanyl to atropine, fentanyl, and mivacurium. Pediatrics 2006; 118 (4): 1583–1591.
Barrington KJ, Byrne PJ . Premedication for neonatal intubation. Am J Perinatol 1998; 15 (4): 213–216.
Cook-Sather SD, Tulloch HV, Cnaan A, Nicolson SC, Cubina ML, Gallagher PR et al. A comparison of awake versus paralyzed tracheal intubation for infants with pyloric stenosis. Anesth Analg 1998; 86 (5): 945–951.
Dempsey EM, Al Hazzani F, Faucher D, Barrington KJ . Facilitation of neonatal endotracheal intubation with mivacurium and fentanyl in the neonatal intensive care unit. Arch Dis Child Fetal Neonatal Ed 2006; 91 (4): F279–F282.
Lemyre B, Cheng R, Gaboury I . Atropine, fentanyl and succinylcholine for non-urgent intubations in newborns. Arch Dis Child Fetal Neonatal Ed 2009; 94 (6): F439–F442.
Lane B, Finer N, Rich W . Duration of intubation attempts during neonatal resuscitation. J Pediatr 2004; 145 (1): 67–70.
Lee HC, Chitkara R, Halamek LP, Hintz SR . A national survey of pediatric residents and delivery room training experience. J Pediatr 2010; 157 (1): 158–161. e153.
Gaies MG, Landrigan CP, Hafler JP, Sandora TJ . Assessing procedural skills training in pediatric residency programs. Pediatrics 2007; 120 (4): 715–722.
Norman E, Wikstrom S, Hellstrom-Westas L, Turpeinen U, Hamalainen E, Fellman V . Rapid sequence induction is superior to morphine for intubation of preterm infants: a randomized controlled trial. J Pediatr 2011; 159 (6): 893–899 e891.
Acknowledgements
This manuscript was first drafted by Dr Crystal Le and reviewed/edited by the coauthors who uniformly approved for submission to The Journal of Perinatology. No funding was needed for this study. There was no honorarium, grant, or any other form of payment given to anyone to produce this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Le, C., Garey, D., Leone, T. et al. Impact of premedication on neonatal intubations by pediatric and neonatal trainees. J Perinatol 34, 458–460 (2014). https://doi.org/10.1038/jp.2014.32
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2014.32
Keywords
This article is cited by
-
Impact of multiple intubation attempts on adverse tracheal intubation associated events in neonates: a report from the NEAR4NEOS
Journal of Perinatology (2022)
-
Practical approaches to sedation and analgesia in the newborn
Journal of Perinatology (2021)
-
Quality assessment and response to less invasive surfactant administration (LISA) without sedation
Pediatric Research (2020)
-
Premedication with neuromuscular blockade and sedation during neonatal intubation is associated with fewer adverse events
Journal of Perinatology (2019)
-
Moving from controversy to consensus: premedication for neonatal intubation
Journal of Perinatology (2018)