Abstract
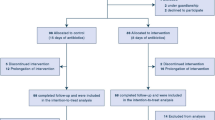
The purpose of this study was to compare the impact of ampicillin and penicillin used for empiric treatment of early onset sepsis (EOS) on initial gut colonization by aerobic and facultative anaerobic microorganisms. A cluster-randomized, two-center, switch-over study was conducted in two paediatric intensive care units in Estonia and included 276 neonates. Rectal swabs were collected twice a week until discharge or day 60. Colonizing microbes were identified on species level and tested for ampicillin resistance (AR). The number of patients colonized with Gram negative microorganisms and Candida spp was similar in both treatment arms but ampicillin resulted in longer colonization duration (CD) of K. pneumonia (p = 0.012), AR Serratia spp (p = 0.012) and Candida spp (p = 0.02) and penicillin in that of AR Acinetobacter spp (p = 0.001). As for Gram positive microorganisms penicillin treatment was associated with a greater number of colonized patients and higher CD of Enterococcus spp and S. aureus but lower ones of S. haemolyticus and S. hominis. Influence of ampicillin and penicillin on initial gut colonization is somewhat different but these differences are of low clinical relevance and should not be a limiting step when choosing between these two antibiotics for the empiric treatment of EOS.


Similar content being viewed by others
References
Donskey CJ (2004) The role of the intestinal tract as a reservoir and source for transmission of nosocomial pathogens. Clin Infect Dis 39:219–226
Sullivan A, Edlund C, Nord CE (2001) Effect of antimicrobial agents on the ecological balance of human microflora. Lancet Infect Dis 1:101–114
Young TE, Mangum B (2004) Neofax: a manual of drugs used in neonatal care. Acorn Publishing, Raleigh
Mehta D (2005) BNF49: British National Formulary. Pharmaceutical Press, Wallingford
Bonnemaison E, Lanotte P, Cantagrel S, Thionois S, Quentin R, Chamboux C, Laugier J (2003) Comparison of fecal flora following administration of two antibiotic protocols for suspected maternofetal infection. Biol Neonate 84:304–310
Stoll BJ, Hansen NI, Higgins RD, Fanaroff AA, Duara S, Goldberg R, Laptook A, Walsh M, Oh W, Hale E (2005) Very low birth weight preterm infants with early onset neonatal sepsis: the predominance of gram-negative infections continues in the National Institute of Child Health and Human Development Neonatal Research Network, 2002–2003. Pediatr Infect Dis J 24:635–639
Gewolb IH, Schwalbe RS, Taciak VL, Harrison TS, Panigrahi P (1999) Stool microflora in extremely low birthweight infants. Arch Dis Child Fetal Neonatal Ed 80:F167–F173
Bennet R, Eriksson M, Nord CE, Zetterstrom R (1982) Suppression of aerobic and anaerobic faecal flora in newborns receiving parenteral gentamicin and ampicillin. Acta Paediatr Scand 71:559–562
de Man P, Verhoeven BA, Verbrugh HA, Vos MC, van den Anker JN (2000) An antibiotic policy to prevent emergence of resistant bacilli. Lancet 355:973–978
Laugel V, Kuhn P, Beladdale J, Donato L, Escande B, Astruc D, Messer J (2003) Effects of antenatal antibiotics on the incidence and bacteriological profile of early-onset neonatal sepsis. A retrospective study over five years. Biol Neonate 84:24–30
Jaureguy F, Carton M, Panel P, Foucaud P, Butel MJ, Doucet-Populaire F (2004) Effects of intrapartum penicillin prophylaxis on intestinal bacterial colonization in infants. J Clin Microbiol 42:5184–5188
Westerbeek EA, van den Berg A, Lafeber HN, Knol J, Fetter WP, van Elburg RM (2006) The intestinal bacterial colonisation in preterm infants: a review of the literature. Clin Nutr 25:361–368
Graham PL 3rd, Della-Latta P, Wu F, Zhou J, Saiman L (2007) The gastrointestinal tract serves as the reservoir for Gram-negative pathogens in very low birth weight infants. Pediatr Infect Dis J 26:1153–1156
Costa SF, Miceli MH, Anaissie EJ (2004) Mucosa or skin as source of coagulase-negative staphylococcal bacteraemia? Lancet Infect Dis 4:278–286
Metsvaht T, Ilmoja ML, Parm U, Maipuu L, Merila M, Lutsar I (2010) Comparison of ampicillin plus gentamicin vs. penicillin plus gentamicin in empiric treatment of neonates at risk of early onset sepsis. Acta Paediatr 99:665–672
Schrag S, Gorwitz R, Fultz-Butts K, Schuchat A (2002) Prevention of perinatal group B streptococcal disease. Revised guidelines from CDC. MMWR Recomm Rep 51:1–22
CLSI (2005) Performance standards for antimicrobial susceptibility testing; fifteenth informational supplement. Clinical and Laboratory Standards Institute, pp 24–25
Brakstad OG, Aasbakk K, Maeland JA (1992) Detection of Staphylococcus aureus by polymerase chain reaction amplification of the nuc gene. J Clin Microbiol 30:1654–1660
Chambers HF (1997) Methicillin resistance in staphylococci: molecular and biochemical basis and clinical implications. Clin Microbiol Rev 10:781–791
Adlerberth I, Lindberg E, Aberg N, Hesselmar B, Saalman R, Strannegard IL, Wold AE (2006) Reduced enterobacterial and increased staphylococcal colonization of the infantile bowel: an effect of hygienic lifestyle? Pediatr Res 59:96–101
Heikkila MP, Saris PE (2003) Inhibition of Staphylococcus aureus by the commensal bacteria of human milk. J Appl Microbiol 95:471–478
Almuneef MA, Baltimore RS, Farrel PA, Reagan-Cirincione P, Dembry LM (2001) Molecular typing demonstrating transmission of gram-negative rods in a neonatal intensive care unit in the absence of a recognized epidemic. Clin Infect Dis 32:220–227
Ronnestad A, Abrahamsen TG, Medbo S, Reigstad H, Lossius K, Kaaresen PI, Engelund IE, Irgens LM, Markestad T (2005) Septicemia in the first week of life in a Norwegian national cohort of extremely premature infants. Pediatrics 115:e262–e268
Schwiertz A, Gruhl B, Lobnitz M, Michel P, Radke M, Blaut M (2003) Development of the intestinal bacterial composition in hospitalized preterm infants in comparison with breast-fed, full-term infants. Pediatr Res 54:393–399
Mammina C, Di Carlo P, Cipolla D, Giuffre M, Casuccio A, Di Gaetano V, Plano MR, D’Angelo E, Titone L, Corsello G (2007) Surveillance of multidrug-resistant gram-negative bacilli in a neonatal intensive care unit: prominent role of cross transmission. Am J Infect Control 35:222–230
Srivastava S, Shetty N (2007) Healthcare-associated infections in neonatal units: lessons from contrasting worlds. J Hosp Infect 65:292–306
Tapiainen T, Ylitalo S, Eerola E, Uhari M (2006) Dynamics of gut colonization and source of intestinal flora in healthy newborn infants. APMIS 114:812–817
Mackie RI, Sghir A, Gaskins HR (1999) Developmental microbial ecology of the neonatal gastrointestinal tract. Am J Clin Nutr 69:1035S–1045S
Edwards RK, Clark P, Sistrom CL, Duff P (2002) Intrapartum antibiotic prophylaxis 1: relative effects of recommended antibiotics on gram-negative pathogens. Obstet Gynecol 100:534–539
Duman M, Abacioglu H, Karaman M, Duman N, Ozkan H (2005) Beta-lactam antibiotic resistance in aerobic commensal fecal flora of newborns. Pediatr Int 47:267–273
Bizzarro MJ, Dembry LM, Baltimore RS, Gallagher PG (2008) Changing patterns in neonatal Escherichia coli sepsis and ampicillin resistance in the era of intrapartum antibiotic prophylaxis. Pediatrics 121:689–696
Mitt P, Adamson V, Loivukene K, Lang K, Telling K, Paro K, Room A, Naaber P, Maimets M (2009) Epidemiology of nosocomial bloodstream infections in Estonia. J Hosp Infect 71:365–370
Bennet R, Eriksson M, Nord CE (2002) The fecal microflora of 1-3-month-old infants during treatment with eight oral antibiotics. Infection 30:158–160
Loivukene K, Kermes K, Sepp E, Adamson V, Mitt P, Jurna M, Magi H, Kallandi U, Otter K, Naaber P (2006) The comparison of susceptibility patterns of Gram-negative invasive and non-invasive pathogens in Estonian hospitals. Antonie Leeuwenhoek 89:367–371
Cassettari VC, da Silveira IR, Dropa M, Lincopan N, Mamizuka EM, Matte MH, Matte GR, Menezes PR (2009) Risk factors for colonisation of newborn infants during an outbreak of extended-spectrum beta-lactamase-producing Klebsiella pneumoniae in an intermediate-risk neonatal unit. J Hosp Infect 71:340–347
Fraser S (2006) Enterococcal infections: eMedicine Specialties. EMedicine, pp 1–18
Miedema CJ, Kerkhof M, Arends JP, Bergman KA, Kimpen JL (2000) Risk factors for colonization with enterococci in a neonatal intensive care unit. Clin Microbiol Infect 6:53
Hufnagel M, Liese C, Loescher C, Kunze M, Proempeler H, Berner R, Krueger M (2007) Enterococcal colonization of infants in a neonatal intensive care unit: associated predictors, risk factors and seasonal patterns. BMC Infect Dis 7:107
Drozenova J, Petras P (2000) Characteristics of coagulase-negative staphylococci isolated from hemocultures. Epidemiol Mikrobiol Imunol 49:51–58
Koksal F, Yasar H, Samasti M (2009) Antibiotic resistance patterns of coagulase-negative staphylococcus strains isolated from blood cultures of septicemic patients in Turkey. Microbiol Res 164:404–410
Arslan S, Ozkardes F (2007) Slime production and antibiotic susceptibility in staphylococci isolated from clinical samples. Mem Inst Oswaldo Cruz 102:29–33
Acknowledgements
The study was supported by Estonian Science Foundation Grant number 6984; Estonian Target Financing number 2726 and ESPID Small Grant Award. The authors are grateful to colleagues from both participating NICUs for their support and help in documenting all clinical decisions, as well as to head nurse Tiina Kilg and all nurses for their help in collecting samples. We would like to thank associated Professor Reet Mändar for her valuable remarks and suggestions while preparing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parm, Ü., Metsvaht, T., Sepp, E. et al. Impact of empiric antibiotic regimen on bowel colonization in neonates with suspected early onset sepsis. Eur J Clin Microbiol Infect Dis 29, 807–816 (2010). https://doi.org/10.1007/s10096-010-0931-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-010-0931-1