Abstract
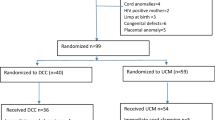
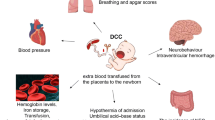
Objective: In a prospective study at Uludag University Hospital, 120 premature infants with birthweights of 1500 g or less were screened for intraventricular hemorrhage (IVH) using cranial ultrasound. With the purpose of studying the incidence of IVH, the associated risk factors for these neonates were considered.Methods : We studied all the very low birth weight infants admitted in our neonatal unit. We examined the following variables as risk factors for IVH: sex, birth weight, gestational age, Apgar score, mechanichal ventilation, hypercapnia, use of antenatal steroids, tocolytic drugs, vaginalversus cesarean section delivery, and inbornversus outborn status, vasopressor infusion (any vasoactive drug such as dopamine, dobutamine, or epinephrine) not associated with resuscitation, and surfactant administration.Results :The incidence of IVH was 15% (18/120), 50% grade I (9/18), 17% grade II (3/18), 11 % grade III (2/18), and 22% grade IV (4/18). IVH occurred mainly in the first week of life (78%; 14/18). The significant risk factors for IVH were found to be prematurity, outborn status, low 5 minute Apgar score, vaginal delivery, hypercapnia, mechanical ventilation, hypotension, and use of vasopressors on the day of admission. Significant protective factors against IVH included antenatal steroid therapy, cesarean section, magnesium sulfate tocolysis, increasing gestational age, and increasing birth weight.Conclusion: Our results concur with the notion that a tertiary center is the optimal location for delivery of the high risk neonate. Transportation of infantsin utero to a perinatal center specializing in high risk-deliveries results in a decreased incidence of IVH when compared to infants transported postnatally. Aggressive resuscitation, with avoidance of hypercarbia, and rapid restoration of hypovolemia could potentially reduce the incidence of PVH/IVH
Similar content being viewed by others
References
Volpe J J.Neurology of the Newborn. 3rd edn. Philadelphia: W.B. Saunders Company; 1995; 424–425.
Papile LA. Incidence and evolution of subependymal and intraventricular hemorrhage. A study of infants with birth weights less than 1500 gm.J Pediatr 1978; 92: 529–534.
Ahmann PA. Intraventricular hemorrhage in high risk premature infants: incidence and outcome.Ann Neurol 1980; 8: 118–124.
Philip AGS. Intraventricular hemorrhage in preterm infants: declining incidence in the 1980’s.Pediatrics 1989; 84: 797–801.
Perlman JM. Intraventricular hemorrhage in extremely small premature infants.Am J Dis Child 1986; 140: 1122–1124.
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1500 grams.J Pediatr 1978; 92: 529–534.
Leviton A. Antenatal corticosteroids appear to reduce the risk of postnatal germinal matrix hemorrhage in intubated lowbirth-weight newborns.Pediatrics 1993; 91: 1083–1088
Vermont-Oxford Trials network. The Vermont-Oxford Trials network: very low birth weight outcomes for 1990.Pediatrics 1993; 91: 540–545.
Funjimura M, Salisbury DM, Robinson ROet al. Clinical events relating to intraventricular haemorrhage in the newborn.Arch Dis Child 1979; 54: 409–414.
Miall-Allen VM, de Vries LS, Whitelaw AG. Mean arterial blood pressure and neonatal ceebral lesions.Arch Dis Child 1987; 62: 1068–1069.
Volpe JJ. Intraventricular hemorrhage in the premature infantcurrent concepts. Part I.Ann Neurol 1989; 25: 3–11.
Bada HS, Korones SB, Perry EHet al. Mean arterial blood pressure changes in premature infants and those at risk of intraventricular hemorrhage.J Pediatr 1990; 117: 607–614.
Synnes AR, Chien LY, Peliowski A, Babolal R, Lee SK. Variations in intraventricular hemorrhage incidence rates among Canadian neonatal intensive care units.J Pediatr 2001; 138: 525–531.
Yu VYH, Bajuk B, Cutting D, Orgill AA, Astbury J. Effect of mode of delivery on outcome of very-low-birthweight infants.Br J Obstet Gynaecol 1984; 91: 633–639.
Ment LR, Oh W, Ehrenkranz RA, Philip AGS, Duncan CC, Makuch RW. Antenatal steroids, delivery mode and intraventricular hemorrhage in preterm infants.Am J Obstet Gynecol 1995; 172: 795–800.
Kuban KC, Leviton A, Pagano M, Fenton T, Strassfeld R, Wolff M. Maternal toxemia is associated with reduced incidence of germinal matrix hemorrhage in premature babies.J Child Neurol 1992; 7: 70–76.
Perlman JM, McMenamin JB, Volpe JJ. Fluctuating cerebral blood-flow velocity in respiratory-distress syndrome. Relation to the development of intraventricular hemorrhage.N Eng J Med 1983; 309: 204–209.
Ilikkan B, Vural M, Yardimci D, Ozbek S, Perk Y, liter O. Intraventricular hemorrhage in preterm newborns.Turk J Pediatr 1998; 40: 195–200.
Greisen G, Trojaborg W. Cerebral blood flow, PaCO2 changes and visual evoked potentials in mechanically ventilated, preterm infants.Acta Paediatr Scand 1987; 76: 394–400
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Köksal, N., Baytan, B., Bayram, Y. et al. Risk factors for intraventricular haemorrhage in very low birth weight infants. Indian J Pediatr 69, 561–564 (2002). https://doi.org/10.1007/BF02722677
Issue Date:
DOI: https://doi.org/10.1007/BF02722677